1918 Influenza Timeline
Introduction
In the end, almost no place was spared. When the Spanish influenza virus circled the world between 1918 and 1919, nearly every place that man had occupied prior to that was affected, with some of the exceptions being islands in the Bering Sea, the northern coast of Iceland, and American Samoa.
Wave 1
Some experts today believe that the virus originated in China—the birthplace of many flu strains. It appears that the virus passed from birds to pigs and then to humans. Its first true victim has been lost to history.
What is known is that on March 11, 1918, an Army cook named Albert Mitchell reported to the infirmary of Camp Funston, Kansas. He had typical flu-like symptoms—a low-grade fever, mild sore throat, slight headache, and muscle aches. He was ordered to rest in bed. By noon of the same day, 107 soldiers at the base were sick with similar symptoms. Within two days, 522 people were sick. Military posts have always been fertile ground for outbreaks of contagious disease. Barracks bring people from many regions into close quarters under high stress. So it wasn't a surprise that ground zero of this outbreak was a military installation, or that the disease was next reported, on March 18, at several Army camps in Georgia. The symptoms were mild, with few deaths. But the numbers of ill were high -- 2,900 cases out of 28,586 troops at the Georgia camps.
The outbreak then hop-scotched from one military post to another in the eastern and southern United States, spilled into the civilian population, and reached the West Coast in late April, where an outbreak was recorded at San Quentin Prison (California).
Influenza hit large cities exceptionally hard: in Philadelphia (Pennsylvania), 158 out of 1,000 people died; 148 out of 1,000 in Baltimore (Maryland); and 109 out of 1,000 in the nation’s capital (Washington, D.C.). The good news (if there was any) was that the disease peaked within two to three weeks after appearing in a given city.
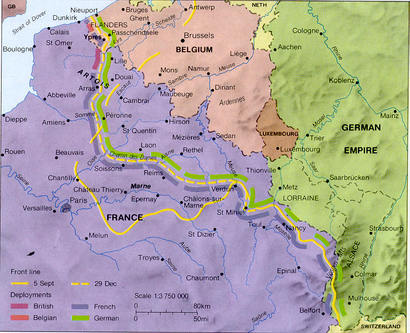
By then, however, it had already made a bigger and more fateful leap, across the Atlantic Ocean with hundreds of thousands of American soldiers going to join the Great War. Outbreaks were noted at an Army camp in Bordeaux, France, and in the port city of Brest, France in early April. By the end of the month it was at the Western Front (see picture below), in the American, British, French and German armies.
In May it arrived in England with troops returning from France. That month saw an outbreak in Madrid, Spain and Seville, Spain that caused a total death rate about twice normal for that time of year. Spain was a neutral country during World War I. Because its news reports were uncensored, the Spanish outbreak received wide publicity. Even at the time, however, experts realized the name "Spanish flu" was entirely misleading as an indicator of the germ's origin.
The outbreak continued to move north and east, getting as far as Scandinavia and Poland. This "spring wave" reached India, arriving in Bombay on May 31 with a troop transport. Puerto Rico, part of the Brazilian coast, Indonesia, Australia and New Zealand experienced outbreaks in June.
Influenza tends to be seasonal, as the virus survives longest in cool, dry air and is most easily spread when people are crowded together -- all conditions favored by winter. It was unusual for the first wave of the 1918 influenza to last as long as it did, and not surprising when things slowed down in August. Then something happened...
In the end, almost no place was spared. When the Spanish influenza virus circled the world between 1918 and 1919, nearly every place that man had occupied prior to that was affected, with some of the exceptions being islands in the Bering Sea, the northern coast of Iceland, and American Samoa.
Wave 1
Some experts today believe that the virus originated in China—the birthplace of many flu strains. It appears that the virus passed from birds to pigs and then to humans. Its first true victim has been lost to history.
What is known is that on March 11, 1918, an Army cook named Albert Mitchell reported to the infirmary of Camp Funston, Kansas. He had typical flu-like symptoms—a low-grade fever, mild sore throat, slight headache, and muscle aches. He was ordered to rest in bed. By noon of the same day, 107 soldiers at the base were sick with similar symptoms. Within two days, 522 people were sick. Military posts have always been fertile ground for outbreaks of contagious disease. Barracks bring people from many regions into close quarters under high stress. So it wasn't a surprise that ground zero of this outbreak was a military installation, or that the disease was next reported, on March 18, at several Army camps in Georgia. The symptoms were mild, with few deaths. But the numbers of ill were high -- 2,900 cases out of 28,586 troops at the Georgia camps.
The outbreak then hop-scotched from one military post to another in the eastern and southern United States, spilled into the civilian population, and reached the West Coast in late April, where an outbreak was recorded at San Quentin Prison (California).
Influenza hit large cities exceptionally hard: in Philadelphia (Pennsylvania), 158 out of 1,000 people died; 148 out of 1,000 in Baltimore (Maryland); and 109 out of 1,000 in the nation’s capital (Washington, D.C.). The good news (if there was any) was that the disease peaked within two to three weeks after appearing in a given city.
By then, however, it had already made a bigger and more fateful leap, across the Atlantic Ocean with hundreds of thousands of American soldiers going to join the Great War. Outbreaks were noted at an Army camp in Bordeaux, France, and in the port city of Brest, France in early April. By the end of the month it was at the Western Front (see picture below), in the American, British, French and German armies.
In May it arrived in England with troops returning from France. That month saw an outbreak in Madrid, Spain and Seville, Spain that caused a total death rate about twice normal for that time of year. Spain was a neutral country during World War I. Because its news reports were uncensored, the Spanish outbreak received wide publicity. Even at the time, however, experts realized the name "Spanish flu" was entirely misleading as an indicator of the germ's origin.
The outbreak continued to move north and east, getting as far as Scandinavia and Poland. This "spring wave" reached India, arriving in Bombay on May 31 with a troop transport. Puerto Rico, part of the Brazilian coast, Indonesia, Australia and New Zealand experienced outbreaks in June.
Influenza tends to be seasonal, as the virus survives longest in cool, dry air and is most easily spread when people are crowded together -- all conditions favored by winter. It was unusual for the first wave of the 1918 influenza to last as long as it did, and not surprising when things slowed down in August. Then something happened...
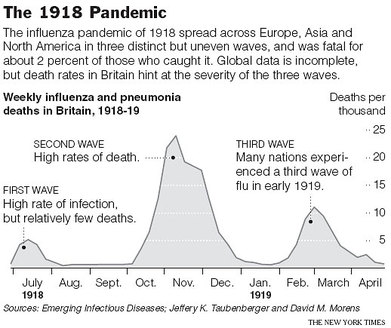
Wave 2
Microbes often adapt and change behavior while epidemics are under way. When slightly different strains are passing from person to person, a strain that kills its victims quickly, before they have time to infect others, may tend to disappear and be replaced by a strain that keeps its victims alive -- and transmitting disease -- for a longer time. There also can be evolutionary pressure for microbes to become more potent, if the change makes their hosts more infectious by, say, loading their mucus with germs or stimulating coughs and sneezes.
In late August 1918 a new outbreak of flu -- the "fall wave" -- began. The virus was as contagious as ever, but now more than 10 times as deadly. Between Aug. 22 and 27, the more potent strain appeared on three continents -- Europe, Africa and North America. The three places -- Sierra Leone's capital, Freetown; Brest, France; and Boston -- were each ports crowded with people coming from distant lands. Of the 2 million American soldiers who went to France in the war, 791,000 landed in Brest. Boston had a shipyard, naval hospital and many agencies shipping war materiel. Freetown was the main coaling station for steamships going from Europe to southern Africa. From these coastal cities the new wave of infection raced to both uninfected territory, such as Africa, and to areas only recently recovered from the spring wave, including Europe and America.
From Boston, the fall wave spread across the United States in six weeks. In Philadelphia, 10,959 people died of influenza in October. Military outposts were again hot spots. Between Sept. 12 and Oct. 11, thirty-seven Army installations suffered outbreaks.
Stanley Lane, who'd given a false birth date on his enlistment papers, was five days shy of his 17th birthday when influenza struck Camp McClellan in Alabama on Sept. 26.
"All I remember about it was I got a little temperature, and I went on sick call and the doctor said, `Go to the hospital, you got the flu,' " he recalled recently at his home in Silver Spring, Maryland.
"When I walked in there the nurse says, `That's your bed over there.'
So I went over and sat down.
And the greetings I got was from all these other GIs around there telling me: `Hey, the guy who just left that bed died,' " Lane, now 101, said with a slight chuckle.
"It didn't bother me. I went to bed.”
He doesn't recall his illness as being especially severe. In any case, he recovered and went on to spend 32 years in the Army, retiring as a lieutenant colonel.
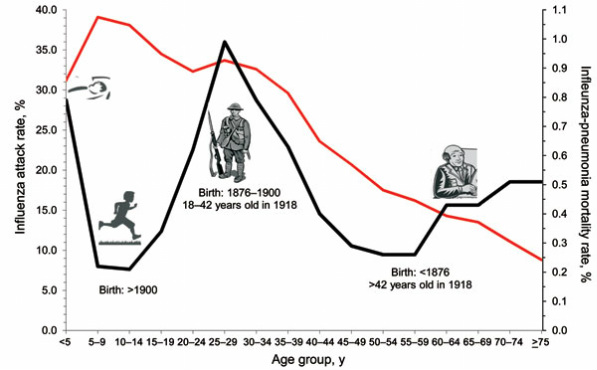
The Spanish flu had an unusual and unexplained preference for young adults, whom it killed in greater numbers than either children or the elderly. Many of Lane's fellow soldiers weren't as lucky as he. About 20,000 died in nine weeks in the United States that fall.
Troops in Europe were rapidly infected as well. The American Expeditionary Forces recorded 37,000 cases of influenza in September -- and 16,000 more in the first week of October. No army was immune. "Influenza gummed up the German supply lines and made it harder to advance and harder to retreat," historian Crosby wrote. "It made running impossible, walking difficult, and simply lying in the mud and breathing burdensome. From the point of view of the generals, it had a worse effect on the fighting qualities of an army than death itself.”
Microbes often adapt and change behavior while epidemics are under way. When slightly different strains are passing from person to person, a strain that kills its victims quickly, before they have time to infect others, may tend to disappear and be replaced by a strain that keeps its victims alive -- and transmitting disease -- for a longer time. There also can be evolutionary pressure for microbes to become more potent, if the change makes their hosts more infectious by, say, loading their mucus with germs or stimulating coughs and sneezes.
In late August 1918 a new outbreak of flu -- the "fall wave" -- began. The virus was as contagious as ever, but now more than 10 times as deadly. Between Aug. 22 and 27, the more potent strain appeared on three continents -- Europe, Africa and North America. The three places -- Sierra Leone's capital, Freetown; Brest, France; and Boston -- were each ports crowded with people coming from distant lands. Of the 2 million American soldiers who went to France in the war, 791,000 landed in Brest. Boston had a shipyard, naval hospital and many agencies shipping war materiel. Freetown was the main coaling station for steamships going from Europe to southern Africa. From these coastal cities the new wave of infection raced to both uninfected territory, such as Africa, and to areas only recently recovered from the spring wave, including Europe and America.
From Boston, the fall wave spread across the United States in six weeks. In Philadelphia, 10,959 people died of influenza in October. Military outposts were again hot spots. Between Sept. 12 and Oct. 11, thirty-seven Army installations suffered outbreaks.
Stanley Lane, who'd given a false birth date on his enlistment papers, was five days shy of his 17th birthday when influenza struck Camp McClellan in Alabama on Sept. 26.
"All I remember about it was I got a little temperature, and I went on sick call and the doctor said, `Go to the hospital, you got the flu,' " he recalled recently at his home in Silver Spring, Maryland.
"When I walked in there the nurse says, `That's your bed over there.'
So I went over and sat down.
And the greetings I got was from all these other GIs around there telling me: `Hey, the guy who just left that bed died,' " Lane, now 101, said with a slight chuckle.
"It didn't bother me. I went to bed.”
He doesn't recall his illness as being especially severe. In any case, he recovered and went on to spend 32 years in the Army, retiring as a lieutenant colonel.
The Spanish flu had an unusual and unexplained preference for young adults, whom it killed in greater numbers than either children or the elderly. Many of Lane's fellow soldiers weren't as lucky as he. About 20,000 died in nine weeks in the United States that fall.
Troops in Europe were rapidly infected as well. The American Expeditionary Forces recorded 37,000 cases of influenza in September -- and 16,000 more in the first week of October. No army was immune. "Influenza gummed up the German supply lines and made it harder to advance and harder to retreat," historian Crosby wrote. "It made running impossible, walking difficult, and simply lying in the mud and breathing burdensome. From the point of view of the generals, it had a worse effect on the fighting qualities of an army than death itself.”
Around the world, wide and cruel variations in mortality were the rule. Poor and marginally nourished people, not surprisingly, fared worst. India lost about 18.5 million people, just less than 6 percent of its population. In the United States, 28% of the population became infected, and 675,000 people died, about 0.7 percent of the population and a figure greater than the amount of American lives lost in all of the 20th-century’s wars. In northern Nigeria, mortality among the general population of white Europeans was 19 per 1,000; among Nigerians, it was 32 per 1,000. Some aboriginal populations were decimated. Mortality in Alaska was horrifying. In one settlement, Brevig Mission, 72 out of 80 natives died in five days, leaving only children and teenagers. The flu was most deadly for young people between the ages of 20 and 40.
Worldwide, it is estimated that anywhere between 20 million and 40 million died. As with SARS today, quarantine was the main tool against Spanish flu. There were no effective medicines. In fact, it wasn't even known that a virus caused the disease. That wouldn’t be discovered until 1933. In general, quarantine worked poorly as it took just one infected person breaking isolation to spread disease. But in one place it worked famously. The Samoan Islands in the Pacific Ocean were split between the United States, which controlled the eastern islands, and New Zealand, which had seized the western islands from Germany at the start of the war. On Nov. 7, 1918, the steamship Talune, from New Zealand, anchored at Apia, the capital of Western Samoa. It carried people ill with flu. "Before the end of that year, a matter of less than two months, 7,542 died of influenza and its complications in Western Samoa, approximately 20 percent of the total population," Crosby writes.
Without orders from the government but based on what he learned from a radio news service, the governor of American Samoa, Navy Cmdr. John Poyer, instituted a quarantine policy. When he heard of the outbreak on Western Samoa, he banned travel to or from the neighboring islands, which were about 40 miles apart. When Western Samoa sent a mail boat to American Samoa, Poyer refused even to allow the bags to be transferred. Poyer persuaded the island's natives to mount a shore patrol to prevent illegal landings. People who disembarked from ships sailing from the American mainland were kept under house arrest for a specified period, or examined daily. Aspects of the quarantine continued into mid-1920, and as a result, were no influenza deaths on American Samoa. Meanwhile, between 80-90% of the Western Samoan population was infected, with many of the afflicted starving to death simply because they were too weak to even feed themselves.
Wave 3
A third wave of Spanish flu began in January 1919, circulating intensively for two months. Although that wave, too, caused many deaths, the virus was running out of victims. The winter of 1920 again saw flu with relatively high death rates. At some point, on a day as lost to history as the one of its emergence, Spanish flu made a final human being ill and then disappeared.
Worldwide, it is estimated that anywhere between 20 million and 40 million died. As with SARS today, quarantine was the main tool against Spanish flu. There were no effective medicines. In fact, it wasn't even known that a virus caused the disease. That wouldn’t be discovered until 1933. In general, quarantine worked poorly as it took just one infected person breaking isolation to spread disease. But in one place it worked famously. The Samoan Islands in the Pacific Ocean were split between the United States, which controlled the eastern islands, and New Zealand, which had seized the western islands from Germany at the start of the war. On Nov. 7, 1918, the steamship Talune, from New Zealand, anchored at Apia, the capital of Western Samoa. It carried people ill with flu. "Before the end of that year, a matter of less than two months, 7,542 died of influenza and its complications in Western Samoa, approximately 20 percent of the total population," Crosby writes.
Without orders from the government but based on what he learned from a radio news service, the governor of American Samoa, Navy Cmdr. John Poyer, instituted a quarantine policy. When he heard of the outbreak on Western Samoa, he banned travel to or from the neighboring islands, which were about 40 miles apart. When Western Samoa sent a mail boat to American Samoa, Poyer refused even to allow the bags to be transferred. Poyer persuaded the island's natives to mount a shore patrol to prevent illegal landings. People who disembarked from ships sailing from the American mainland were kept under house arrest for a specified period, or examined daily. Aspects of the quarantine continued into mid-1920, and as a result, were no influenza deaths on American Samoa. Meanwhile, between 80-90% of the Western Samoan population was infected, with many of the afflicted starving to death simply because they were too weak to even feed themselves.
Wave 3
A third wave of Spanish flu began in January 1919, circulating intensively for two months. Although that wave, too, caused many deaths, the virus was running out of victims. The winter of 1920 again saw flu with relatively high death rates. At some point, on a day as lost to history as the one of its emergence, Spanish flu made a final human being ill and then disappeared.